I always discuss the need to stay one step ahead of the bladder in MS with my patients, as having a urinary tract infection (UTI) can mimic a relapse and cause real setbacks.
Explain this to your GP, request they prescribe antibiotics at the first sign of infection, and that NICE guidelines recommend a longer (5–10-day) course for these ‘neurogenic’ UTIs. It’s also worth taking at least a prescription away with you on holiday to prevent losing days trying to see a doctor.
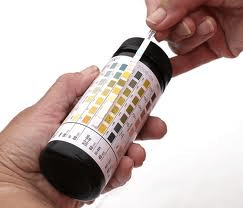
Check! Whenever you experience new or worse symptoms of MS, always check for a silent UTI. Aswell as visiting your surgery or MS nurse, you can also buy urinalysis dipsticks for home use. A change of colour to Leukocytes or Nitrites may indicate infection, which should be treated.
If you take antibiotics, top up with probiotics (good bacteria), during and afterwards, to prevent digestive problems and thrush, and boost your health and resistance to future UTIs. Lactose-free capsules or powder are better than sweet probiotic drinks. In fact looking after the good bacteria in your gut is a huge and important topic for all of us, and particularly if you have an auto-immune condition, and there’s lots of ways you can do this.

Also drink plenty of water, pee frequently, and cut out sugar to help your immune system fight back.
Causes.
One cause of UTIs with MS is the bladder not emptying fully, because the muscles involved are not working together properly. Struggling to start passing urine, feeling there’s some left, urgency, and UTIs can all be signs of incomplete emptying. This needs to be identified by ultrasound scan, generally with the continence service.

Try peeing twice every time, but if a residual (left over) volume of 100mls or more is found, you may need to learn how to use intermittent self-catheterisation with small, lubricated, disposable catheters, to empty fully.
ISC can be liberating, but also potentially cause infection; technique and catheter type are important, so stay in touch with your advisor.

Prevention and natural treatments
If you seem to keep getting urine infections one after the other, it’s quite likely that you are just not completely throwing off one infection.
It’s a very dispiriting situation, However – there are lots of things you can do to shake off and help prevent recurrent UTIs.
The most common bacteria causing UTIs is E coli, which can cause recurrent UTIs, as it can burrow into the bladder wall, and release spores after antibiotics are finished. However, it’s important that your urine goes to the lab, as rarer bugs are also possible, including from candida, which we’re not covering here today. GPs are recommended not to prescribe low dose daily antibiotics, but they sometimes help as a last resort.
Sometimes antibiotic treatment no longer seems to work, or some people prefer to try herbal remedies with antibiotic properties. Stopping the bacteria from sticking to the bladder wall and flushing it out when it does is the aim of these natural agents. There are many, with varying degrees of research to back them, but the ones that I have seen most success with are: (Nb I don’t get any benefit from these companies!)
For prevention:
- Concentrated cranberry tablets, eg Cysticlean
http://www.cysticlean.co.uk/main/index.php
For prevention ( low dose) and/or treatment ( full dose)
- D-Mannose; a simple sugar that e-coli latches on to and can be flushed out on, and is now being tried by consultants at the national hospital for neurology and neurosurgery. https://www.waterfall-d-mannose.com/dmannose-options.html

- SOS advance; a colloidal solution of antibiotic herbs that can be used preventatively or at times of infection.
http://www.sosessentials.com/s/

For recurrent UTIs with an indwelling catheter
If after a catheter changes, with symptoms, ask District Nurses to test from the port after 48 hours, and have an antibiotic at the ready; test again 48 hours after completion.
The ‘Bardex IC’ ( infection control) silver tipped catheter has been shown to reduce UTIs, (reports infections 3.7 x more common in those catheterised with a normal catheter vs a sliver tipped one) as it prevents a biofilm forming. It becomes effective after around 3 months ( and has to be changed regularly like all indwelling catheters), so don’t give up too soon.

If all else fails, ask for a referral to urology, to check for bladder stones, and possibly for bladder washout, and to discuss possible treatments.
See a doctor if you have a fever, chills, pain in the flank area, nausea or vomiting, and always check any natural/herbal remedies are safe to take with your condition and medications.
UPDATE: – I thought this comment from Jenny was important enough to update the blog with:
“I thought I’d let you know about some other treatments for UTIs that are being tried on me that no-one seems to know about (not even doctors in Oxford, nor the MS specialist nurses – I’m keeping them posted too)..
So one is Uromune, supposedly a vaccination against four strains of UTI including e-coli. It’s inactivated bacteria taken in pineapple juice under the tongue once a day for 3 or 6 months. They’re doing a trial in Reading and there are details here http://www.readingurologypartnership.com/uti-vaccine/4594063839 – you can’t get on the trial if you self-catheterise but can pay privately for it (not cheap – including seeing the consultant it was about £600 for me).
And the other is iAluRil, a GAG layer replacement, which you stick inside directly with a catheter, to replenish the non-stick lining of the bladder, and keep in for as long as poss (I do it at night and sleep with it in – it’s only 50mls). There are apparently two places in the UK which don’t do this and Oxford is one, so I go to the Royal Berks for that, on the NHS. Info here http://ialuril.co.uk/
Apologies if you knew all this and that just took up time that you’ll never get back! But I thought, if you don’t know about it, you’re the sort of person who will be interested and use the info to help people. (btw I have no financial links to any of the organisations – am just a person with MS and RUTIs who’s trying everything!). And also I should let you know that I’ve been on the Uromune for nearly 3 months now and just had an e-coli infection… hey ho.”
–Dear Jenny – this is fab; I’m going to post it up as an update so everyone can see, thankyou. I do have a patient who was on the immunisation trial but unfortunately it did not work for her. The aAlUril I have never heard of and am going to look into. Thanks again for your most useful comments!
all the best, Miranda
