I’d forgotten about this article until I needed to find the references to stress for a piece of work I’m doing.But I’m quite proud of it, and I still use HeartMath alot in clinical practice, so here it is, courtesy of the MS Trust, where it was first published
.http://www.mstrust.org.uk/professionals/information/wayahead/articles/15022011_07.jsp
and here it is , but without the long list of references:
Using the HeartMath technique to reduce stress in people with MS
Miranda Olding, MS Specialist Nurse
Bedford MS Therapy Centre
Way Ahead 2011;15(2):12-13
Miranda Olding was the clear winner of the poster prize at the 14th Annual MS Trust Conference for her work on stress management. In the following article, Miranda expands on the project she carried out.
Introduction
From the first recorded medical observations of MS, a link has been noted between stress and MS. Charcot, who first described MS as a disease, cited ‘prolonged grief’, financial problems, and ‘circumstances of moral order’ as being associated with the appearance of symptoms1. More recently, a close association between stress and MS relapses has been found by many researchers2,3,4. In one study in patients with MS, experience of at least one stressful event during a period of four weeks was associated with double the risk of an exacerbation within the next week5. Not all researchers agree however6,7,8. Some of this discrepancy may be due to the different methods and the types of stress recorded – for example in Nisipeanu’s study8, the life threatening acute stress experienced by the subjects who were exposed to the threat of daily missile attacks in the Persian Gulf War in 1991 seemed to have a protective effect on their MS.
The controversy over stress as a trigger factor for MS disease activity has prompted many literature reviews, and a meta analysis published in the BMJ in 20049 concluded that there is a consistent association between stressful life events and subsequent exacerbation in multiple sclerosis. The authors go on to caution that this should not be used to infer that patients are responsible for their exacerbations, but rather they hope that the findings would lead to the development of new behavioural or pharmacological strategies to combat the stress-relapse link.
How could stress promote relapses in MS and how can quality of life be improved?
At least one study in people with MS has shown that reducing distress can reduce the T-cell production of pro-inflammatory cytokines associated with relapse10. Animal studies suggest that an increase in cortisol, the hormone produced during stress, leads to an increase in the permeability of the blood brain barrier and increased inflammation through the release of tumour necrosis factor-alpha, histamines, and tryptase11,12. On a seesaw with cortisol is the hormone dehydroepiandrosterone (DHEA). Feelings of wellbeing, happiness, contentment and appreciation lead to increased levels of DHEA in the bloodstream, which are associated with better sleep, increased energy, a slower aging process and a reduction in inflammatory activity13.
In 2010, Wollin et al14 reported that the one factor that impacted most on quality of life in MS, over and above disease severity and duration, as measured by the WHOQOL-100 instrument, was ‘self-efficacy’ – the ability to do things oneself to help overcome life’s challenges.
What is HeartMath?
The HeartMath technique is a simple breathing and positive emotion technique, it needs no equipment or lengthy training to practise and master. It is taught using biofeedback to record and display heart rate variability (HRV) on a computer screen so clients are immediately able to see the changes in the autonomic nervous system that result from its use. Using HeartMath on a regular basis has been shown to increase positive emotion, decrease depression and anxiety, reduce cortisol levels and increase levels of DHEA15,16.
The field of neurocardiology believes that the heart, rather than being simply a mechanical pump for blood, has its own nervous system, and not only receives but also transmits complex patterns of neurological, hormonal, pressure and electromagnetic information to the brain and throughout the body17. Negative emotions lead to disorder in heart rate variability patterns and in the autonomic nervous system, adversely affecting the rest of the body. In contrast, positive emotions create increased harmony and coherence in heart rhythms and improve balance in the nervous system. Dramatic positive changes occur when techniques are applied that increase coherence in rhythmic patterns of heart rate variability. These include shifts in perception, the ability to reduce stress and deal more effectively with difficult situations, heightened mental clarity, improved decision making and increased creativity and positive feeling18.
Background and aim of research
I became interested in using the HeartMath technique with my patients, after hearing about its use in education and because I see many people who attribute current or recent worsening of their MS to stressful life events, or to feeling stressed. It also appealed to me as it is a drug free strategy which people can manage themselves. The aim of this research was to find out whether using Heartmath could reduce stress in people with MS, with a long term aim of helping to reduce MS disease activity.
Method
The study involved 20 clients (17 women, 3 men) with MS (aged 19-63) who believed that stress was, or had recently been exacerbating their MS. The participants (13 with relapsing remitting MS and seven with secondary progressive MS) had identified stress as a trigger factor for relapse, worsening, or an ongoing problem, associated with their MS. They were offered HeartMath training and gave their informed consent to take part in the research.
A Hospital Anxiety & Depression Score (HADS) was taken as a baseline measurement. This was followed by one session of HeartMath training, which took approximately 15 minutes. Participants were instructed to practise the technique for a minimum of ten minutes at the start of each day, but also at any time when they felt anxious or agitated, found themselves mentally free, or were trying to get to sleep. Most of the HeartMath training sessions were integrated into a general clinic appointment with the MS nurse. Within a three month timescale, participants had a follow up appointment or were contacted by telephone to repeat the HAD score and record any qualitative comments.
Results
Of the 20 participants, 15 used HeartMath regularly, one used it occasionally, two did not use it at all, and two were not followed up within the three month time period. Of the HeartMath regular user group, 100% had improved HAD scores. In the whole group, three had worsened HAD scores.
In the HeartMath regular user group, the average initial HAD score was 20.1 (severe anxiety/depression), on review the average score was 13.6 (moderate anxiety/depression). The average reduction on the HAD score was 7.06 points.
Qualitative data was all positive, with statements recorded including:
“I’m sleeping better, six hours instead of four.”
“I actually feel the benefits of it, and it is something that I know I can do myself.”
“I know my scores didn’t change much, but this year, it is amazing that I’m not worse.”
“I don’t think people who knew me five years ago would even recognise me, how I react to things now.”
Discussion
This was a very small and informal trial, with no control group. Both the intervention and data collection were carried out by the same investigator, which could have introduced unconscious bias in the responses. There were many variables some people whose first HAD score was ‘very stressed’ went on to try many different approaches, including changes to their medications, jobs and activities. So their reduced HAD scores may not necessarily only be due to the use of HeartMath.
However, there were also people who within the timescale of the trial suffered redundancy or job instability, relapse or physical problems due to MS. They commented that they felt that using HeartMath had helped them to retain emotional equilibrium during these difficulties. Some improvement to mood may result solely from the listening and support that comes about when taking part in a trial. However, the results indicate significant changes which suggest that HeartMath has a role to play as a safe, effective holistic intervention for stress in people with MS. It was feasible for the HAD score to be assessed and the HeartMath technique to be taught within ‘normal’ MS clinic appointments, in which other problems were also addressed.
- For more information about HeartMath, see www.heartmath.org
- For info on using HeartMath personally or with clients in the UK, email Miranda Olding
Conclusion and recommendations
Stress is a recognised trigger factor for exacerbations in MS. In this study, teaching the self- management technique HeartMath with regular home practice was associated with an average decrease of 7.06 points on the HAD scale. The intervention was time and cost-effective, and a range of positive effects were noted. It would be useful to replicate the findings in controlled studies and to ask the question: Can relapses or disease activity in MS be reduced by reducing stress?’
References
And, because I’m still searching and turning stuff up, here’s the peice that was published by the HeartMath people, to add to their resources!
|
|
|
|

English Nurse Uses HeartMathWith Multiple Sclerosis Patients
A nurse in England who specializes in patients with multiple sclerosis/MS conducted an informal study in which patients with the disease achieved significant reductions in stress after practicing a HeartMath technique.
Study participants who practiced HeartMath’s Quick Coherence® Technique, which uses heart breathing and focusing on positive emotions, realized an average point drop of more than 30% on the Hospital Anxiety Depression (HAD) Scale, nurse Miranda Olding said.
 Miranda Olding, MS Specialist Nurse, England “I have begun to use HeartMath routinely in my MS special nurse clinic, as stress is a known trigger for relapses in MS,” said Olding, who conducted her study from November 2009 through August 2010 with patients at the MS Therapy Centre in Bedford, England. “My clients with MS respond really positively, I enjoy sharing the skill, and the research I carried out backs up its clinical effectiveness.”
“Stress is a recognized trigger factor for exacerbations in MS,” Olding wrote in the conclusion of her study, Using the HeartMath Technique to Reduce Stress in People With MS. “In this study, teaching (a HeartMath self-management technique) with regular home practice was associated with an average decrease of 7.06 points on the HAD scale.
“The intervention was time and cost effective, and a range of positive effects were noted. It would be useful to replicate the findings in controlled studies, and to ask the question: ‘Can relapses or disease activity in MS be reduced by reducing stress?’”
Olding, a licensed biofeedback practitioner and licensed HeartMath provider who is interested in integrated medicine using conventional and holistic techniques, has written articles about her research for magazines in the United Kingdom. She explains in her research report what led her to conduct the trials.
“I became interested in using the HeartMath technique with my patients after hearing about its use in education, and then using it myself, because I see many people who attribute current or recent worsening of their MS to stressful life events, or to feeling stressed,” she said. “It also appealed to me as a drug-free strategy which people can do themselves. The aim of my research was to find out whether using HeartMath could reduce stress in people with MS, with a long-term aim of helping to reduce MS disease activity.”
The belief that stress affects MS is not a new one.
“From the first recorded medical observations of MS,” Olding wrote, “a link has been noted between stress and MS. (Jean-Martin) Charcot, who first described MS as a disease, cited ‘prolonged grief’ financial problems, and ‘circumstances of moral order’ as being associated with the appearance of symptoms.’” (While Charcot, 1825 – 1893, a French neurologist and pioneer in neurology, is not alone in making a connection between stress and MS, Olding noted in her report that there is still skepticism about such a connection in the medical community.)
 Olding’s study included three men and 17 women from the ages of 19 and 63, all of whom “believed that stress was, or had recently been exacerbating their MS.” The patients who believed stress was a “trigger factor” for a relapse or worsening of their MS symptoms consented to participating in HeartMath training. Olding’s study included three men and 17 women from the ages of 19 and 63, all of whom “believed that stress was, or had recently been exacerbating their MS.” The patients who believed stress was a “trigger factor” for a relapse or worsening of their MS symptoms consented to participating in HeartMath training.
“They were instructed to practice the technique for at least 10 minutes a day (first thing), but also at any time when they felt anxious or agitated, found themselves mentally free, or were trying to get to sleep,” Olding said, noting that 15 of the participants actually used HeartMath regularly.
“Although some reduction in anxiety and depression might be expected to result from the support of a nurse specialist, the drop in HAD scores in the HeartMath user group was consistent and significant enough to suggest that this technique was effective in lowering anxiety and depression as a result of stress in people with MS.”
Research over the last 22 years by the Institute of HeartMath has shown that focusing on positive emotions such as gratitude or appreciation, compassion and caring can help increase an individual’s heart rate variability pattern, or coherence. Coherence is a highly beneficial state in which the heart, mind and emotions are in energetic alignment and cooperation. Coherence builds resiliency.
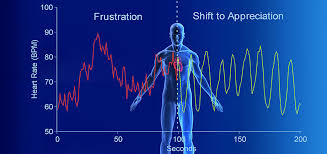
 IHM Director of Research Rollin McCraty explains: “Heart rate variability (HRV), a measure of how responsive the heart is to tiny chemical changes in the bloodstream, stimulating the heart to beat or relax, is directly affected by emotion. Negative emotion such as frustration or anger cause a low or incoherent HRV pattern, and positive emotions such as gratitude cause a high HRV pattern.” IHM Director of Research Rollin McCraty explains: “Heart rate variability (HRV), a measure of how responsive the heart is to tiny chemical changes in the bloodstream, stimulating the heart to beat or relax, is directly affected by emotion. Negative emotion such as frustration or anger cause a low or incoherent HRV pattern, and positive emotions such as gratitude cause a high HRV pattern.”
Olding stressed that her trial group was relatively small, the research was informal and she had no control group. She said there were many variables in the trial, including changes in medication, jobs and activities by participants who had scored high on initial, or baseline stress tests. These people tried numerous other approaches in the process, so all of the variables could have contributed to the final HAD scores.
Nevertheless, she noted, “The results indicate significant changes which suggest that HeartMath has a role to play as a safe, effective holistic intervention for stress in patients with MS. … Of the HeartMath regular user group, 100% had improved HAD scores.”
Olding shared comments from participants in the regular HeartMath user group made after the study.
- “Brilliant. Absolutely helped me so much. It’s made such a massive difference.”
- “I’m sleeping better – six hours instead of four.”
- “I actually feel the benefits of it, and it is something that I know I can do myself.”
- “I know my scores didn’t change much, but this year, it is amazing that I’m not worse.”
- “I don’t think people who knew me five years ago would even recognize me, how I react to things now.”
|



 Connecting with others and having their support defuses this feeling, so tell other people who care about you, and let them know how they can help you through.
Connecting with others and having their support defuses this feeling, so tell other people who care about you, and let them know how they can help you through.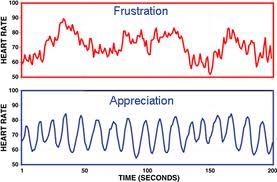











 It hasn’t worked for everyone that’s tried it; it seems to be more effecitve for fatigue in relapsing remitting, rather than progressive MS, and we are still collecting data about this, but the therapy is available privately ( see ‘my other work’ button) and at 7 MS Therapy Centres:
It hasn’t worked for everyone that’s tried it; it seems to be more effecitve for fatigue in relapsing remitting, rather than progressive MS, and we are still collecting data about this, but the therapy is available privately ( see ‘my other work’ button) and at 7 MS Therapy Centres:




 Miranda Olding, MS Specialist Nurse, England
Miranda Olding, MS Specialist Nurse, England Olding’s study included three men and 17 women from the ages of 19 and 63, all of whom “believed that stress was, or had recently been exacerbating their MS.” The patients who believed stress was a “trigger factor” for a relapse or worsening of their MS symptoms consented to participating in HeartMath training.
Olding’s study included three men and 17 women from the ages of 19 and 63, all of whom “believed that stress was, or had recently been exacerbating their MS.” The patients who believed stress was a “trigger factor” for a relapse or worsening of their MS symptoms consented to participating in HeartMath training. IHM Director of Research Rollin McCraty explains: “Heart rate variability (HRV), a measure of how responsive the heart is to tiny chemical changes in the bloodstream, stimulating the heart to beat or relax, is directly affected by emotion. Negative emotion such as frustration or anger cause a low or incoherent HRV pattern, and positive emotions such as gratitude cause a high HRV pattern.”
IHM Director of Research Rollin McCraty explains: “Heart rate variability (HRV), a measure of how responsive the heart is to tiny chemical changes in the bloodstream, stimulating the heart to beat or relax, is directly affected by emotion. Negative emotion such as frustration or anger cause a low or incoherent HRV pattern, and positive emotions such as gratitude cause a high HRV pattern.”